Introduction
The Shoulder and elbow Surgery Unit can host 11 patients, located in 4 rooms with private bathroom. 4 operating sessions are performed weekly and one session of day surgery is performed monthly. The ward doctor is present every day from 7.30 am to 1.30 pm. The ward round is performed twice a week (Monday and Thursday). At least two nurses assist patients in the ward. The senior nurse is present from Monday to Saturday between 7 am and 1 pm.
Clinical practice
The Shoulder and Elbow Surgery Unit was created in 2000, with the aim of focusing attention and energies in pathologies of shoulder and elbow.
The activity of the ward is almost fully dedicated to the cure of pathologies of shoulder (rotator cuff tears, recurrent dislocation and articular laxity, primitive and secondary osteoarthritis, humeral fractures, scapula and clavicular fractures, acromioclavicular and sternoclavicular dislocations, malunion or nonunion), elbow (fractures and luxations, articular instabilities, arthritis, primitive or post-traumatic stiffness, malunion or nonunion) and forearm (fracture, malunion, instability like Essex-Lopresti syndrome).
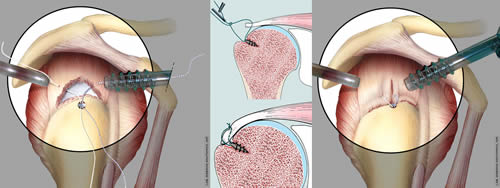
Conflict syndromes, cuff ruptures and articular instability of the shoulder are treated by arthroscopy according to the most innovative techniques (with micro-screws and dedicated instruments), with the help of open field surgery in those cases when the best result cannot be guaranteed by arthroscopy. The instruments and devices are the most innovative, like, when possible, full-wire anchors, reabsorbable or radio transparent anchors.
In the same way, elbow arthroscopy is performed for loose bodies removal, in the treatment of arthritic or post-traumatic stiffness, in the treatment of cartilaginous pathologies (as osteochondritis dissecans in young sports people) and in the treatment of some particular intra-articular fractures (radial head, capitulum humeri or coronoid process), siding without substituting open surgery.
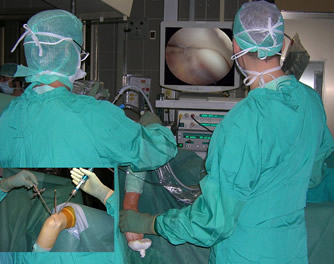
Advanced degenerative-arthritic diseases of shoulder and elbow are treated by prosthetic replacement with the aim of providing pain free movement in elderly patients or in younger patients with severe post-traumatic joint diseases.
In the latest years, articular shoulder and elbow prostheses intensely developed, with always more “anatomic” designs (that is, systems that are similar to the anatomy of the healthy joint).
The continuous research in minimally invasive and new materials development allow us, when indicated, to use implants with short stem or pyrocarbon surfaces, solutions that allow to better respect the patient's anatomy and the osteo-cartilaginous structures of the shoulder, with the aim to speed up the post operative recovery and reduce the possible complications.
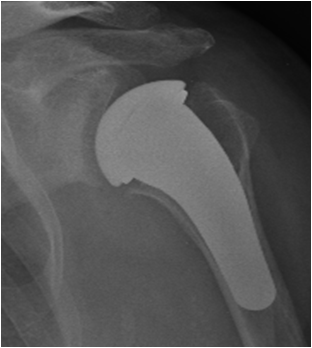
Patients with an irreparable rotator cuff tear (who, until recently, have been severely limited in their activities) can today be treated with the so-called “inverse prosthesis”, which is based on the inversion of the articular surfaces shape.
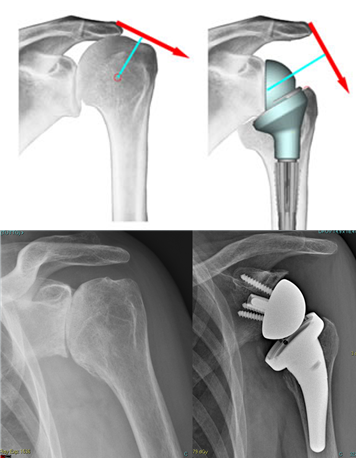
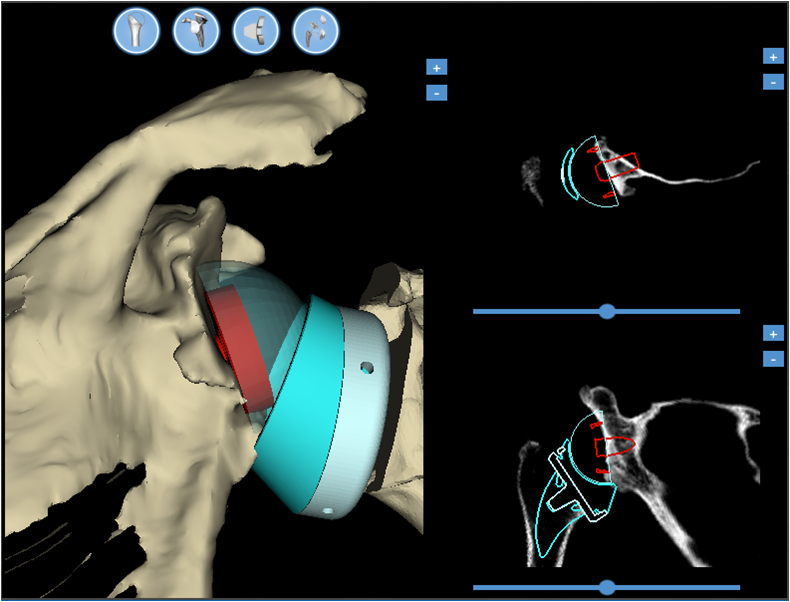
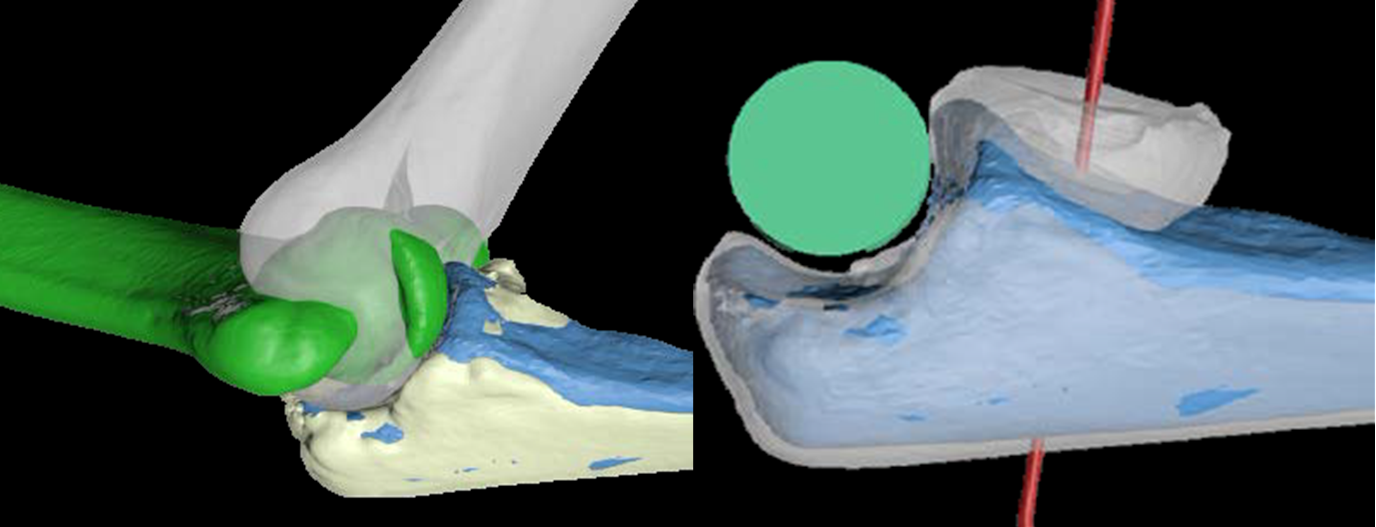
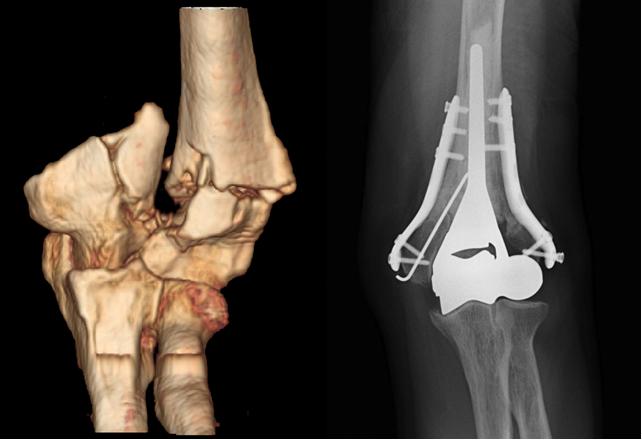
Hardware for traumas was also developed (endomedullary systems, more resistant and better contoured titanium plates, which provide an improved strength of the screw-bone and screw-plate interface, plates made of xray-transparent plastic material, fig. 4), up to providing bioreabsorbable screws, useful in some rare articular fracture.
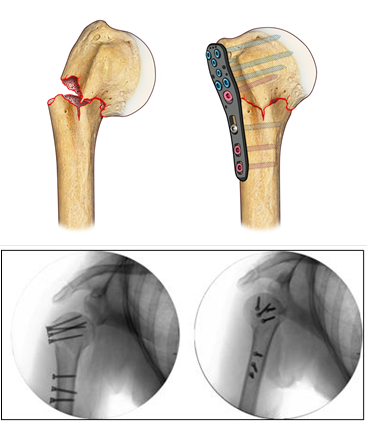
In most severe cases, when it is not possible to reduce and fix the elbow intra-articular fracture, a prosthesis substitution (of the joint humeral part) and a synthesis with plates and screws can be necessary, contemporarily, within the same surgical session.
Nonunions or malunions are often treated with associating metal plates with bone grafts (from donors) and growth factors (platelet gel produced from the patient’s blood), thanks to the presence, within the Institute, of the transfusion service and the Musculoskeletal Tissue Bank.
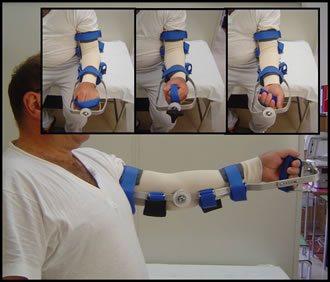
A special attention is dedicated to an early rehabilitation, with the aid of braces (fig. 6) and dedicated motorized devices, as well as of advanced techniques of continuous loco-regional anesthesia, which allows a painless joint mobilization.
Research activity
 From its foundation, the Shoulder and Elbow surgery Unit continuously performs teaching and research activity. It participates to several national and international clinical studies, for example for the ultrasound guided treatment of calcific tendinopathy, the development of new materials for osteosynthesis of shoulder and elbow fractures, for the insertion of shoulder arthroplasty in the Italian register of Orthopedic prosthetic Implant (RIPO). Several patents have been ideated and registered, such as a titanium mini-plate for surgical repair of the rotator cuff, a special postoperative brace for the shoulder, a self-threading titanium screw for a plastic plate.
From its foundation, the Shoulder and Elbow surgery Unit continuously performs teaching and research activity. It participates to several national and international clinical studies, for example for the ultrasound guided treatment of calcific tendinopathy, the development of new materials for osteosynthesis of shoulder and elbow fractures, for the insertion of shoulder arthroplasty in the Italian register of Orthopedic prosthetic Implant (RIPO). Several patents have been ideated and registered, such as a titanium mini-plate for surgical repair of the rotator cuff, a special postoperative brace for the shoulder, a self-threading titanium screw for a plastic plate.
The Unit has a constant partnership with scientific laboratories to improve arthroscopic suture techniques in rotator cuff repair, for shoulder prosthesis design improvement, and in the field of regenerative medicine for poor quality or massive tears of rotator cuff tendons, for the study and treatment of osteoporosis.
The teaching activity is performed with the continuous organization of courses and conferences on shoulder and elbow pathology, with updates in diagnostic, surgical and rehabilitation state-of-the-art techniques, with the participation of national and international guests. In particular, the “Rizzoli Advanced Elbow Surgery Course”, the “Elbow factors” focused on rehab, both biannual; collaboration with the 1st level master on “upper limb surgery”, organized by the University of Bologna. During these activities, state of the art technologies are used, like the use of 3D educational surgical movies, in order to provide a better visualization of the anatomical structures.
The continuous training of the Unit’s personnel is realized also through the active participation to several national and international courses and conferences, often as speakers or moderators.
Staff
Contacts and Locations
Secretary's Office
phone +39-051-6366482
(Mon-Fri, 9 to 10 am)
fax +39-051-6366188
e-mail segreteria.multispec@ior.it
Rizzoli Orthopaedic Institute
via G.C.Pupilli, 1
40136 Bologna (Italy)