Introduction
Keywords: osteoarthrosis, rheumatoid arthritis, partial and total joint replacement, hip/knee/ankle prostheses, ligament reconstruction, surgical techniques, bone preparation guides, patient specific instrumentation, pre-operative planning, medical imaging, bone computer models, prosthesis design, personalized prostheses, 3D-printing, Selective Laser Melting, joint mobility and stability, experimental assessment, in-silico / in-vitro / in-vivo, natural and replaced joint, joint motion and stiffness, surgical navigation, robot assisted surgery, mobilization and loosening.
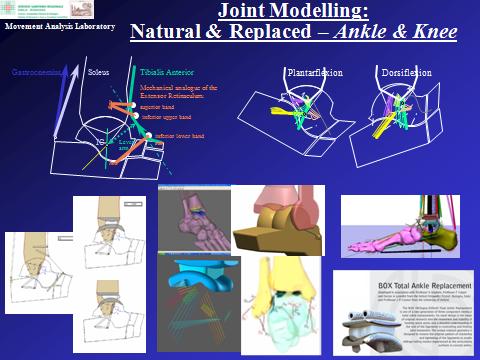
Modelling intact and replaced joints
Computer musculo-skeletal-ligamentous models support the comprehension of human joint mechanics, and the relevant design of prosthetic replacements; these have been developed in the Laboratory to accomplish the instrumental measures, particularly for complex joints, such as the knee and ankle. These models can simulate the effects of traumas or surgical operations, and provide a useful aid to the interpretation of relevant measurements. In addition, joint kinematic and dynamic models have contributed notably to the design of new joint prostheses. These designs were based for the first time on detailed knowledge of the complex mechanism which guides mobility of the lower limb joints, a mechanism formed likewise from articular surfaces and ligaments. Models of the intact and replaced joints are continually tested in in-vitro experiments, to assess their ability to restore normal joint function. A new type of ankle prosthesis (BOX Ankle, Finsbury, UK) was designed and tested in the Laboratory, and is now implanted in a large number of orthopaedic centres internationally. The corresponding operative technique was demonstrated to be very efficient, and the final clinical results are very satisfactory. A number of prototypes for total knee and ankle replacements are under development and test. A most recent activity addresses the design and test of custom-made prosthesis, for patient-specific solutions in joint replacement, also with the utilisation of modern 3D printing facilities.
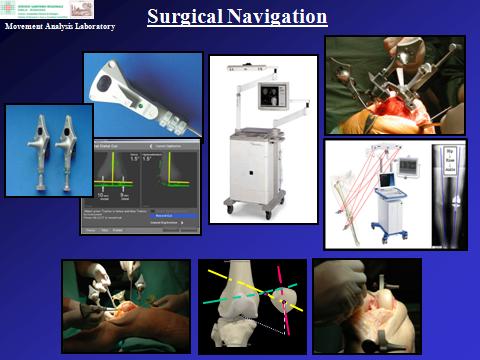
Surgical navigation
This modern technique is an important tool for surgeons during the operation, allowing a more precise execution of most surgical actions (aligning, sawing, drilling, etc.) by enhancing standard direct vision of the patient with geometrical-anatomical-functional information in real-time in the operating theatre. This is achieved typically by simple sets of sterilizable clusters of markers connected rigidly with bone segments and with the surgical tools used, tracked in space by a system of digital cameras which do not hinder the standard surgical procedures. The intra-operative surgical navigation is also used in connection with pre-operative computer based planning, and particularly post-operative research activities in the Laboratory, by providing, during the surgery, fundamental information on the replaced joint, in terms of geometry of the implant and other anatomical structures, for more complete post-operative analyses of the patients. Randomized studies are being carried out in our Lab on the performance of these navigation systems in the operating room, as well as accuracy and repeatability studies. These systems are also used in in-vitro investigations to analyse ligament elongation patterns and joint modelling. An important and original series of studies investigated the traceability and navigability of the patella during knee navigation surgery, taking a new overall procedure from in-vitro feasibility to clinical studies.
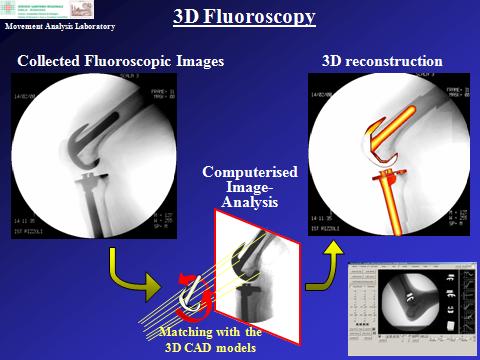
Three-dimensional Videofluoroscopy
Over the years, traditional movement analysis has been integrated with advanced three-dimensional tools for measuring kinematics at replaced joints by means of videofluoroscopy. These techniques allow 3D monitoring, during motor tasks typical of daily living or special extreme exercises, of the relative position and orientation of the implanted prosthetic components respectively with one millimetre and one degree accuracy. This has been exploited in a number of different two- and three-component designs of hip, knee and ankle prostheses; in fact, in addition to the tracking of the metal components affixed to the bone, also the polyethylene inserts in between can be tracked by means of additional small markers. 3D fluoroscopy can be used also in combination with traditional gait analysis and radiostereometry.
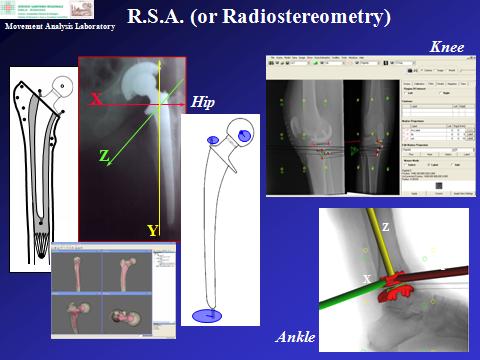
Radiostereometry
Also the measure of the relative prosthesis-to-bone movement is available, known as radiostereometry (or Roentgen-Stereophotogrammetric-Analysis, or RSA). Early identification of this micro-movement, along the course of the patient follow-up, has been shown to result in prosthesis component mobilisation and eventually in failure of the joint replacement, i.e. implant loosening. Small markers are inserted in the prosthetic components and in the corresponding bone at the time of surgery, and their positions are tracked with high accuracy by dual standard radiographic exposures of the replaced joint. It is another accessible tool to assess new implant performance in real patients, particularly to identify their success or failure well in advance. The technique is applied successfully for hip, knee, and ankle joint prostheses.