Introduction
The Movement Analysis Laboratory was established in 1989 as an independent research unit of the Rizzoli Orthopaedic Institute, with the purpose of performing quantitative instrumental analysis of human movement, in particular of the locomotor apparatus. The Laboratory, in close collaboration with the 1st Orthopaedic and Traumatologic Clinic and other Rizzoli clinical units, is specialized in gait analysis both in normal and pathological subjects, mostly in patients before and after surgery or following special rehabilitations programs.
A team of engineers, physiatrists and surgeons, works with a high-level of integration in a large number of movement-science projects and clinical studies, also by assisting and supervising the research activities of residents from the Faculty of Engineering, Medicine and Surgery, Specialization Schools in Orthopaedics, Physical Medicine and Rehabilitation, as well as students on the degree course for Podiatry, Orthopaedic Technicians and Physiotherapists. For many of the past and current projects, strong international collaborations have been established with renowned institutions, universities, and companies.
The Laboratory takes advantage of state-of-the-art instrumentation for the objective measurement of human motion, via stereophotogrammetry or Inertial Measurement Units (IMU), and of the internal and external forces generated through human movement, via force- and pressure-plates and EMG systems. These instruments allow accurate tracking of the kinematics and dynamics of the body segments, and of the relevant joints involved in the motor task under investigation.
The laboratory activities are focused on three main areas of interest:
- Kinematic and dynamic analysis of human movement;
- Joint prostheses;
- Foot orthotics and footwear.
The aspects of movement that are mainly developed during the Laboratory practice involve methodological research and basic biomechanics and clinical research. The Laboratory is actively working, therefore, both in the design and verification of experimental protocols standardized for gait analysis and clinical evaluations of orthopedic and neurological patients. These are sent to the Laboratory within the scope of clinical collaborations, research projects, or industrial commissions.
One of the main aims of the Movement Analysis Laboratory is to understand fully the reasons for the success or failure of orthopedic surgical operations or rehabilitation treatments. These reasons must be identified and distinguished in each type of implant, different surgical techniques, and also single patients. This is of great benefit to the improvement of the techniques currently used and the design of new ones. It is by now known that the real outcome of these operations have to be assessed on the patients, in vivo, after the implant, and in daily living activities, in addition to the standard in-vitro pre-implant tests.
The mission of the Laboratory of Movement Analysis and Functional-Clinical Evaluation of Prosthesis is achieved by the following two main general actions:
- research-healthcare integration;
- research-teaching integration.
Research-healthcare integration
The objectives that the laboratory aims to achieve are the following:
- to be a reference centre for the functional evaluation of patients with diseases of the locomotor apparatus, for diagnostic and therapeutic purposes;
- to identify clearly, even in the early phase of the clinical experimentation, the single numerical parameters best predicting a possible failure of the prosthetic implants. These parameters, to be monitored during the patient follow-up, can be based on in-vivo measurements of the patient via motion analysis techniques, or the result of advanced biomechanical analyses or computer model simulations;
- to be a reference centre for the design and testing of movement analysis protocols, for these to be transferred and used in other clinical contexts both in orthopaedics and rehabilitation centres.
Research-teaching integration
The continuous interaction with medical and bioengineering students allows for a very strong synergy between research and teaching. The Laboratory is the ideal place for scientific studies and collaborations with public and private institutions, which support biomedical research according to known guidelines. The availability of highly specialized instruments, and the continuous interaction of the research team with national and international scientific communities, support the development of educational material which is of great communicative value for programmes in medicine, bioengineering and physiotherapy.
Main research activities:
Keywords (general): biomechanics of locomotion, functional recovery, medical device, joint replacements, design - assessment – validation - efficacy, joint rotations and moments, patents, clinical studies, musculoskeletal models, computer model simulations, cloud-computing, orthopaedic surgery, flat foot, ageing, personalized treatments, sport/performance, bioengineering, physical rehabilitation, occupational medicine.
Research Activity
Keywords: gait analysis, stereophotogrammetry, baropodometry, dynamometry, electromyography, inertial sensors, instrument validation, protocol design, sport/performance, functional recovery, ergonomics, biofeedback, rehabilitation/exercise at home.
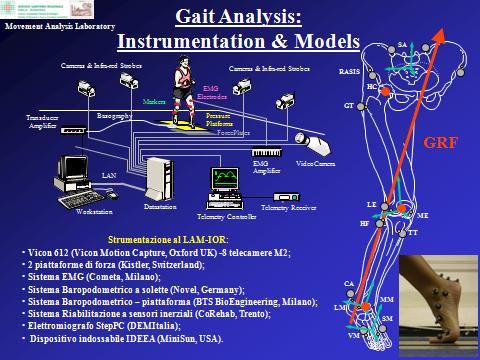
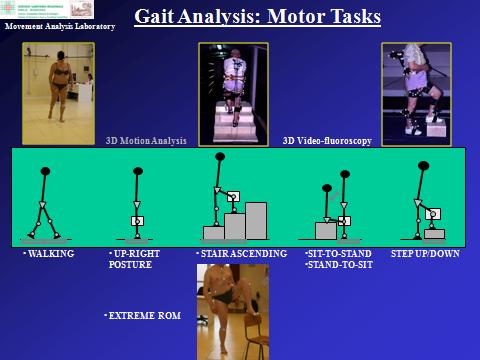
The Laboratory uses, designs and tests state-of-the-art technology in the field of "gait analysis". Advanced instruments enable the non-invasive acquisition, during normal tasks of daily living, of the three-dimensional position of small markers attached to the body segments, of the ground reaction force and of the muscular activity, from which kinematics and dynamics of the major joints are calculated. The motor tasks analysed include, but are not limited to: walking, ascent/descent of stairs, sitting/rising from a chair, ascent/descent of a step, squat, lunge, and upper limb reaching. Common lower-limb and upper-limb rehabilitation exercises are also analysed.
The instruments available to the laboratory comprise two stereophotogrammetric systems, for a total of 14 high-frequency cameras, two high-speed video cameras, a 16-channel surface wireless EMG, two force plates, instrumented pressure insoles, a pressure platform, a set of Inertial Measurement Units (IMU), and a foot scanner. Relevant measurements are integrated and synchronized, for consistent and time-synchronized datasets. All analyses are minimally-invasive, and are performed in a short time by experienced staff with no risk associated to the subject.
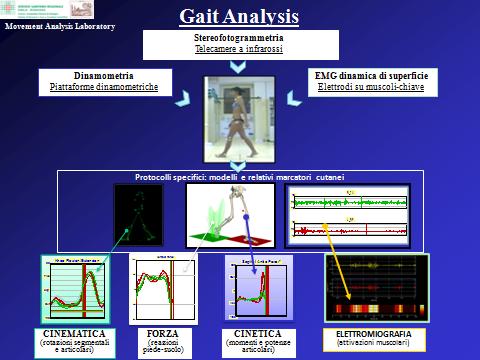
Novel kinematic protocols and corresponding biomechanical models have been designed by the team of engineers and physiatrists of the Laboratory. Some of these are wide-spread within the scientific and gait-analysis communities, which have appreciated the accuracy, repeatability and interpretability of the relevant motion analysis results, and these protocols have recently become international standards. These techniques have been applied successfully to several parts of the human body, such as the upper limb, the trunk and spine, and the foot, and exploited in a number of pathological and normal/control populations, possibly before and after treatments. These can be surgical, pharmacological, physical, including also orthotics interventions such as joint orthosis, brace, splint, and insole, for ankle, knee, column, shoulder, elbow and wrist.
Keywords: osteoarthrosis, rheumatoid arthritis, partial and total joint replacement, hip/knee/ankle prostheses, ligament reconstruction, surgical techniques, bone preparation guides, patient specific instrumentation, pre-operative planning, medical imaging, bone computer models, prosthesis design, personalized prostheses, 3D-printing, Selective Laser Melting, joint mobility and stability, experimental assessment, in-silico / in-vitro / in-vivo, natural and replaced joint, joint motion and stiffness, surgical navigation, robot assisted surgery, mobilization and loosening.
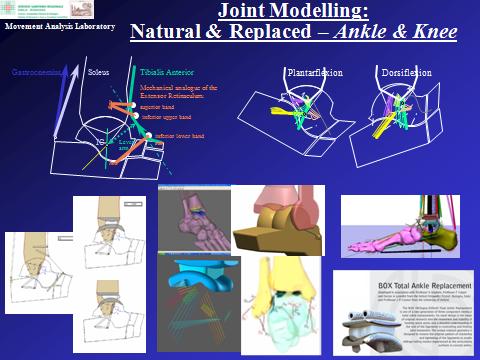
Modelling intact and replaced joints
Computer musculo-skeletal-ligamentous models support the comprehension of human joint mechanics, and the relevant design of prosthetic replacements; these have been developed in the Laboratory to accomplish the instrumental measures, particularly for complex joints, such as the knee and ankle. These models can simulate the effects of traumas or surgical operations, and provide a useful aid to the interpretation of relevant measurements. In addition, joint kinematic and dynamic models have contributed notably to the design of new joint prostheses. These designs were based for the first time on detailed knowledge of the complex mechanism which guides mobility of the lower limb joints, a mechanism formed likewise from articular surfaces and ligaments. Models of the intact and replaced joints are continually tested in in-vitro experiments, to assess their ability to restore normal joint function. A new type of ankle prosthesis (BOX Ankle, Finsbury, UK) was designed and tested in the Laboratory, and is now implanted in a large number of orthopaedic centres internationally. The corresponding operative technique was demonstrated to be very efficient, and the final clinical results are very satisfactory. A number of prototypes for total knee and ankle replacements are under development and test. A most recent activity addresses the design and test of custom-made prosthesis, for patient-specific solutions in joint replacement, also with the utilisation of modern 3D printing facilities.
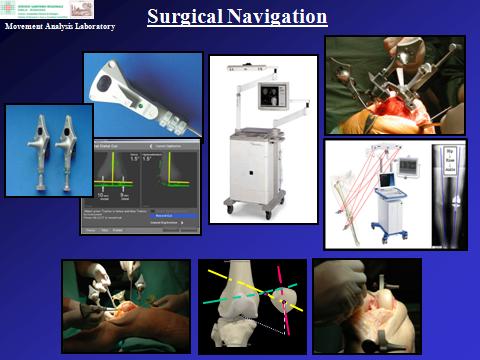
Surgical navigation
This modern technique is an important tool for surgeons during the operation, allowing a more precise execution of most surgical actions (aligning, sawing, drilling, etc.) by enhancing standard direct vision of the patient with geometrical-anatomical-functional information in real-time in the operating theatre. This is achieved typically by simple sets of sterilizable clusters of markers connected rigidly with bone segments and with the surgical tools used, tracked in space by a system of digital cameras which do not hinder the standard surgical procedures. The intra-operative surgical navigation is also used in connection with pre-operative computer based planning, and particularly post-operative research activities in the Laboratory, by providing, during the surgery, fundamental information on the replaced joint, in terms of geometry of the implant and other anatomical structures, for more complete post-operative analyses of the patients. Randomized studies are being carried out in our Lab on the performance of these navigation systems in the operating room, as well as accuracy and repeatability studies. These systems are also used in in-vitro investigations to analyse ligament elongation patterns and joint modelling. An important and original series of studies investigated the traceability and navigability of the patella during knee navigation surgery, taking a new overall procedure from in-vitro feasibility to clinical studies.
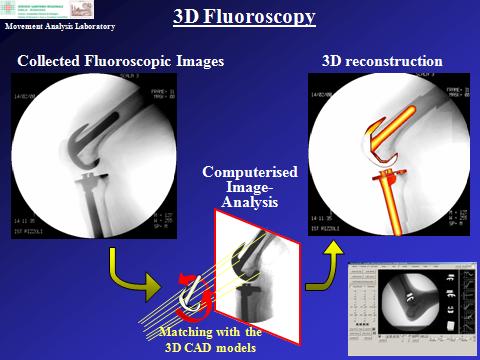
Three-dimensional Videofluoroscopy
Over the years, traditional movement analysis has been integrated with advanced three-dimensional tools for measuring kinematics at replaced joints by means of videofluoroscopy. These techniques allow 3D monitoring, during motor tasks typical of daily living or special extreme exercises, of the relative position and orientation of the implanted prosthetic components respectively with one millimetre and one degree accuracy. This has been exploited in a number of different two- and three-component designs of hip, knee and ankle prostheses; in fact, in addition to the tracking of the metal components affixed to the bone, also the polyethylene inserts in between can be tracked by means of additional small markers. 3D fluoroscopy can be used also in combination with traditional gait analysis and radiostereometry.
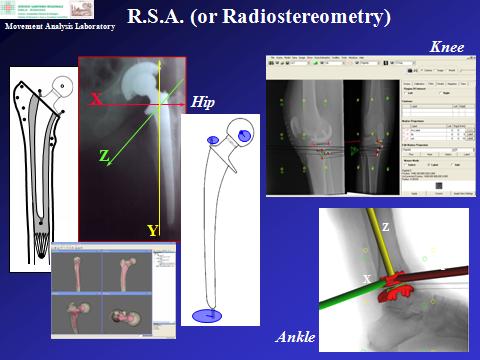
Radiostereometry
Also the measure of the relative prosthesis-to-bone movement is available, known as radiostereometry (or Roentgen-Stereophotogrammetric-Analysis, or RSA). Early identification of this micro-movement, along the course of the patient follow-up, has been shown to result in prosthesis component mobilisation and eventually in failure of the joint replacement, i.e. implant loosening. Small markers are inserted in the prosthetic components and in the corresponding bone at the time of surgery, and their positions are tracked with high accuracy by dual standard radiographic exposures of the replaced joint. It is another accessible tool to assess new implant performance in real patients, particularly to identify their success or failure well in advance. The technique is applied successfully for hip, knee, and ankle joint prostheses.
Keywords: foot biomechanics, foot pathologies, multi-segment foot kinematics, insoles, orthopaedic shoes, ankle-foot orthoses, braces / splints, personalized orthosis, instrumented insoles, diabetic foot, overloading, plantar pressure, industrial boots / safety shoes, podoscope, 3D scanner, 3D printing.
Areas of research:
- Joint Orthosis (foot and ankle, knee, trunk, elbow, wrist)
- Orthopaedic Shoes
- Orthopaedic, functional, and sport insoles
Foot orthotics, such as insoles and ankle-foot orthoses, are special devices for the support, alignment and correction of the foot and lower limb joints. These devices can be made with single or composite materials and can be produced with different technologies. The prescription of the most appropriate foot orthotics requires, first, in-depth assessment of the ailment or pathology that must be addressed in order to restore the normal kinematic alignment of the anatomical segments. Different combinations of technologies and materials can be designed to provide the mechanical solution to the patient’s problems. While traditionally the design of orthotic devices were based on the experience of a few professional technicians, it is now becoming increasingly important to apply the latest technologies for the personalization or mass-customization of the device. Moreover, these devices require highly sophisticated instrumentation and expertise for the objective functional assessment of lower limb biomechanics.
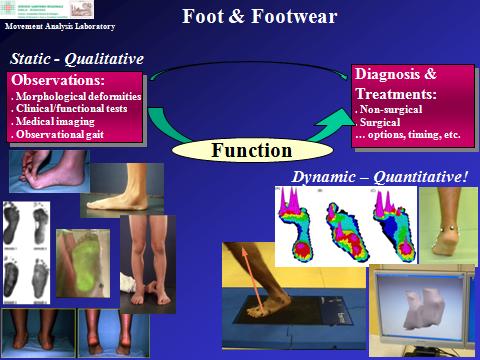
The “Feet & Footwear” technical group, a team of engineers and clinicians within the Movement Analysis Laboratory with strong background in foot biomechanics and foot pathologies, has the whole set of necessary expertise to assess, design and analyse the patients ailment from the diagnosis to the prescription of current devices or design of novel solutions, which can include insoles, shoes, and also rehabilitation and surgical treatments.
The major aims of the group are the following:
- improving the quality of life for the patients (e.g. with flat/cavus foot, diabetic, rheumatic, elderly, paediatric, oncologic, sport professionals and workers);
- advancing the current knowledge on foot biomechanics and pathology, and on the foot/orthotics biomechanical interaction;
- supporting the industry either by assessing current technologies and products, or by devising novel technological solutions.
In addition to standard gait analysis instrumentation, specific tools and devices are employed to assess the kinematics and kinetics of the foot and ankle complex. These include one pressure plate, one podoscope, one 3D foot laser scanner, and all-size 99-sensor instrumented insoles for baropodometric measures. Original methodologies, such as the close integration between pressure and kinematic data, have been originally implemented to improve our understanding of foot biomechanics, in normal and pathological conditions. In addition, custom software have been developed specifically for the automatic and precise analysis and processing of pressure-plate and instrumented-insole measurements.
Some of our past and current activities with industrial partners include:
- baropodometric assessment of military boots;
- thorough functional assessment of forefoot offloading shoes;
- evaluation of single-rocker shoes;
- plantar pressure in personalized insoles for professional soccer players;
- assessment and testing of CLOUD-based technologies for the design of custom-insoles in safety shoes;
- design and test of women high-heel shoes.
Overall, the availability and the ability to work with all these techniques allow to make progresses over the entire process and follow the entire story of the treatment implying medical devices, from the original pre-operative planning, to the assessment of efficacy, up to the design of possible novel devices.

Staff



Contacts and Locations
Secretary's office
phone +39-051-6366571
fax +39-051-6366561
Rizzoli Orthopaedic Institute
Research Center Codivilla-Putti
via di Barbiano, 1/10
40136 Bologna (Italy)


